Data from Scotland’s COVID vaccination programme has revealed a possible small increase in the risk of a treatable and often mild bleeding disorder after the first dose of the Oxford/AstraZeneca vaccine.
Doctors examined the medical records of 5.4 million people in Scotland for instances of blood clots, unusual bleeding, and a condition called idiopathic thrombocytopenic purpura (ITP), where a reduction in blood platelets can lead to easy bruising, bleeding gums and internal bleeding.
The analysis conducted with Public Health Scotland found the risk of ITP was marginally higher in the 1.7 million people who had received a first dose of the Oxford/AstraZeneca vaccine than in a comparison group that did not receive the shot up to 14 April, 2021.
Writing in Nature Medicine, the researchers estimate there are an additional 11 cases of ITP for every million doses of the Oxford/AstraZeneca vaccine administered. The side-effect is mostly observed in older people with chronic health problems such as coronary heart disease, diabetes or chronic kidney disease, and typically appears from the second to fourth week.
The increased rate of ITP after the Oxford/AstraZeneca shot is similar to that seen with other vaccines such as the flu, MMR and hepatitis B jabs, where 10 to 30 additional cases of ITP occur per million doses.
Catching the coronavirus itself carries a substantially higher risk of ITP. The study found weaker evidence for an increased risk of clots in the arteries and bleeding events after the AstraZeneca vaccine.
There was no sign of a greater risk from ITP, clotting or bleeding in the 800,000 people in Scotland who had received the Pfizer/BioNTech Covid vaccine up to 14 April.
“Overall, this is pretty reassuring,” said Aziz Sheikh, a senior author on the study and professor of primary care research and development at the University of Edinburgh. “At the population level, we are seeing low risks from the vaccine and there are treatments for people who develop ITP.”
In May, the Joint Committee on Vaccination and Immunisation (JCVI) advised that under-40s should receive an alternative to the Oxford/AstraZeneca Covid vaccine given the low levels on infection in the United Kingdom (UK) and the very rare risk of a potentially serious condition called vaccine-induced thrombosis and thrombocytopenia or VITT.
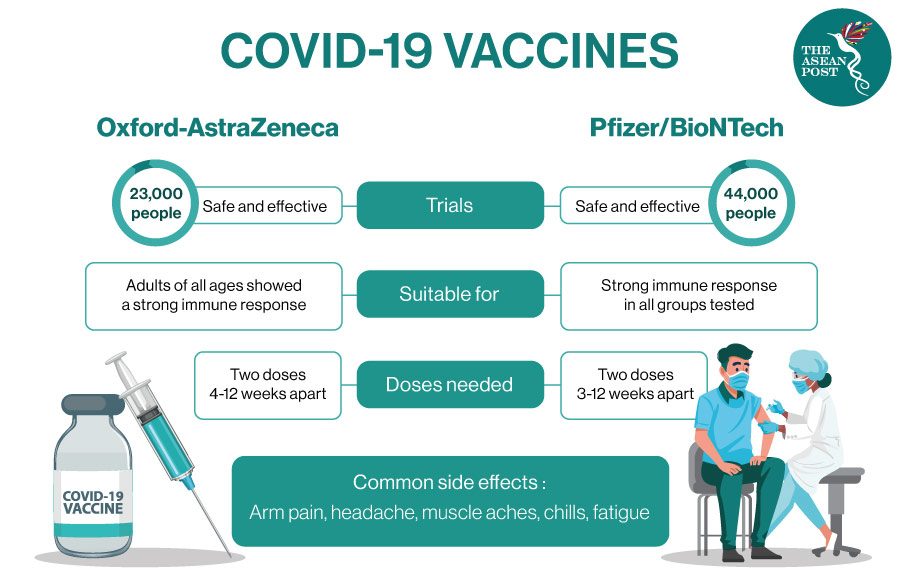
In line with that advice, most under-40s in the UK now receive either the Pfizer/BioNTech or Moderna jabs, which are based on a different technology to the Oxford/AstraZeneca shot.
Treatments For ITP
“If people experience bruising or bleeding after the Oxford/AstraZeneca vaccine, it is important to let their GP know because there are good treatments available for ITP,” Prof Sheikh said. “The wider message is that the risk of these outcomes is much lower with the vaccine than if you develop COVID-19.”
Stephen Evans, a professor of pharmacoepidemiology at the London School of Hygiene & Tropical Medicine, said ITP developed in about 340 per 100,000 people who developed COVID. “Even if the Oxford/AstraZeneca vaccine does have an increased risk of ITP, its benefit outweighs its risk. For the majority of people ITP does not cause serious problems, but it is not the case for everyone.”
Adam Finn, a professor of paediatrics and member of JCVI at the University of Bristol, said ITP was often diagnosed when no other cause for low blood platelets could be found. “It may cause bleeding and treatments are available to prevent this but in many cases the condition is mild and self-limiting,” he said.
“Overall, this study adds somewhat to the understanding of the haematological problems that occur in very small numbers of recipients of this vaccine and, given its importance to the global effort to control the pandemic, ongoing efforts to clarify the characteristics, causes and mechanisms of these events are extremely important,” he added. – The Guardian